 Mike McSherry, CEO and co-founder of Xealth
Mike McSherry, CEO and co-founder of Xealth
A little while back, my friend’s 82-year-old father had hip replacement surgery, which went well and after a few days of recovery, he was eager to get home. He was discharged late in the evening and by that time, the local home medical equipment (HME) store was closed and so he went home without a walker. His wife would pick one up in the morning.
In the middle of the night, he got up to use the restroom and fell.
Of course he re-injured his hip and ended up back in the hospital for additional treatment that could have been avoided if the things he needed to recover had been simply delivered to him prior to the procedure.
I recently had the opportunity to share this experience during a presentation at the HME News Business Summit in Cleveland. It is amazing to me, in the day of Amazon, Walmart, Instacart, and BestBuy’s Geek Squad bringing nearly anything imaginable to our front doors, that we have to wait for a brick-and-mortar storefront to open in the morning to get medical equipment. There was a lot of discussion about how the HME space will evolve over the year to take advantage of new technologies, new service delivery capabilities, rapid consolidation of players, and new large entrants to the space.
Evolving expectations of payors, employers, physicians, health systems and most importantly, patients will change how supplies and equipment get to patients to help them recover and stay healthy. This presents tons of new opportunities for HMEs and physicians to make sure patients have everything they need before it is critical – if they are nimble enough to figure this out and act on it before someone else does.
The payment ecosystem is evolving with patients shouldering a heavier burden of their healthcare costs. Insurance plans are not the only consideration, and people have to ask if it is cheaper to pay for equipment through a health savings account instead of through the plan. At what point is it covered – a week before the procedure? The day after surgery? When??
Remote patient monitoring services are becoming mainstream to track blood pressure, heart rhythm, and A1c levels. These devices are spitting out data that could be fed back to the physician in an intelligent way that informs care decisions and allows for early interventions, as needed, without becoming information overload.
Additional revenue may also be generated for primary care with HMEs supplying remote patient monitoring tools up front. They can also be reimbursed by payor for compliance, catching people before they get sick again.
The digitization and internet of things offers a real opportunity for HME vendors and the surrounding ecosystem to further drive revenue and efficiency. The last decade has taught us that consumers expect both customization and convenience. They will order five versions of an item online, knowing they will send back four of them. There is no longer the need to see and feel something in person before making a purchase. That presents a challenge to any vendor that does not offer an online or service-related extension of their traditional storefront. At the same time, service matters.
Digital health tools are enabling digital therapeutics and remote patient monitoring initiatives, and helping facilitate partnerships, including those between payors, device manufacturers, providers, supply chain partners and HMEs. Compliance can be monitored and e-mails to patients triggered, improving the care journey supporting value-based contracts. Usage data can be used to support health systems and HMEs to negotiate more results driven (and compensated) payor agreements.
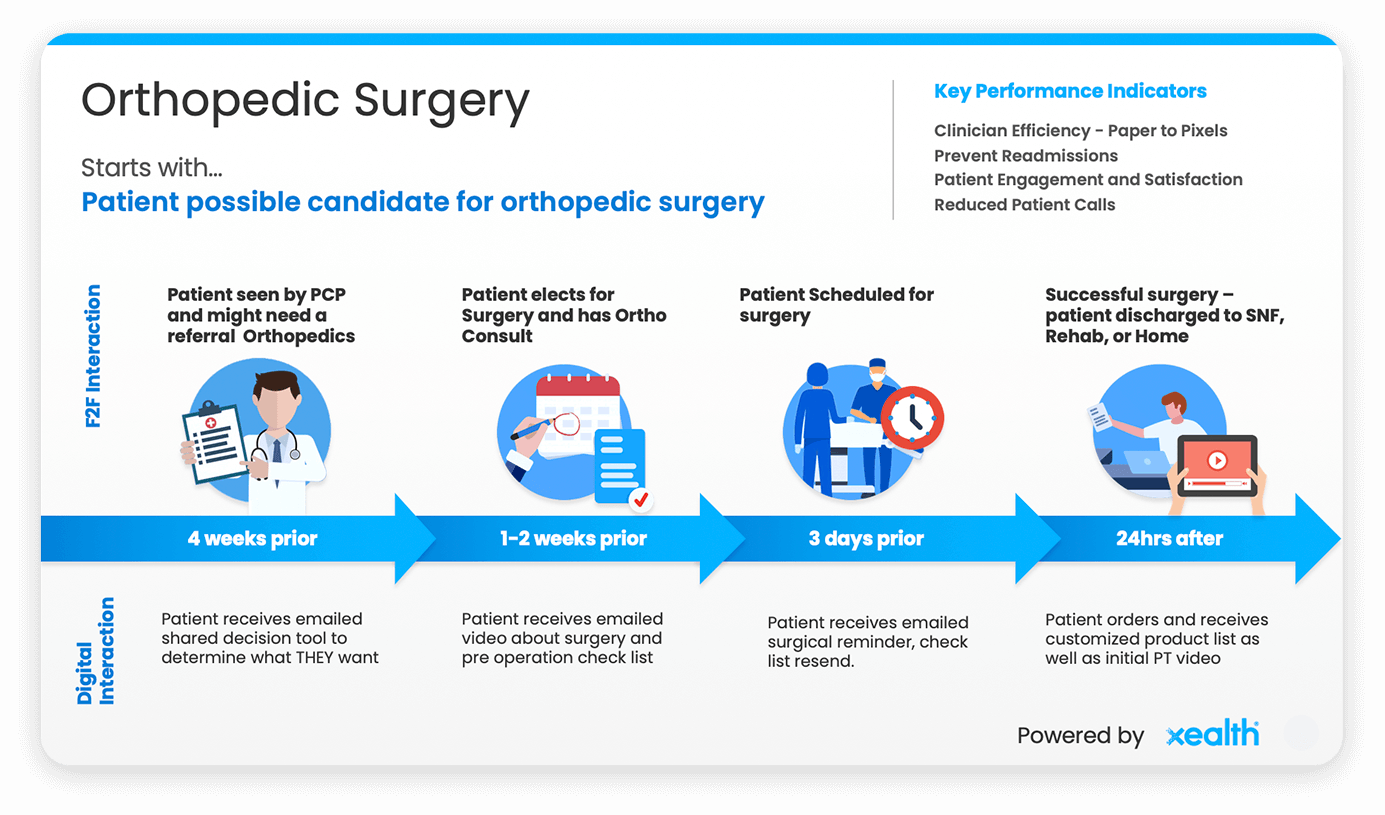
Imagine the story with the hip replacement again. This time, the health system triggers digital health engagement based on the scheduled surgery feed. First, education is e-mailed, informing the patient what to expect and what is needed to prepare and recover. The day prior, a walker and other assets appear at the door, so the patient is ready to recover safely at home. The evening before the surgery, a reminder message is sent with operating day instructions – when to arrive, when to stop eating or drinking, etc. Maybe a ride service such as Lyft is scheduled if the patient does not have reliable transportation. Following surgery, another alert is triggered for physical therapy to schedule an appointment. All of this is done without extra work and now the patient is set, not just for the procedure, but also to return home.
This is the care delivery story we should be telling, with technology facilitating a partnership along the ecosystem for a better experience. A balance needs to be struck between today’s storefronts and tomorrow’s technology, and how digital health care can enable a better patient experience, a lower administrative burden for providers, and supply evidence for hospital administrators on what is working.


